Explore this overview of radiation therapy to get a better understanding of the prostate cancer treatment at the Advanced Prostate Cancer Institute.
Continue readingShould women be afraid to visit a urologist? – Dr. Nicole Szell
Women may feel apprehensive about visiting a urologist due to its personal nature. Learn more from Dr. Szell, urologist in Palm Harbor, FL.
Continue readingWhat are Dr. Yaser Bassel’s specialties in urology?
Dr. Bassel main interest is robotic surgery in urology, which allows for precision and minimally invasive treatment of cancer-related issues.
Continue readingWho is Dr. Brian Hale and what is his approach to screening for prostate cancer?
According to Dr. Hale, all men over the age of 50 should be screened for prostate cancer to avoid any serious complications in the future.
Continue readingWhat is the diagnosis and treatment for prostate cancer by Dr. David Harris?
The first step in diagnosing prostate cancer is obtaining a biopsy, which provides crucial information. Learn more from urologist, Dr. Harris.
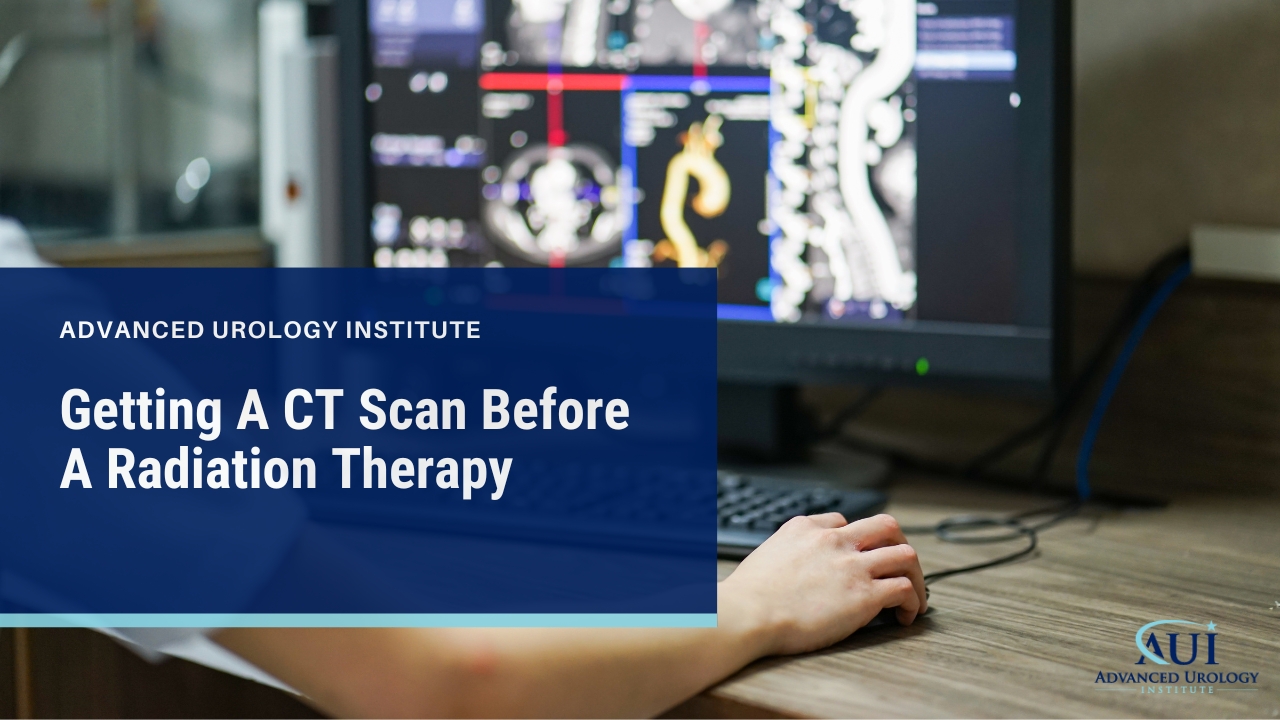
Continue readingGetting A CT Scan Before A Radiation Therapy
Fred, a radiation therapist at Advanced Prostate Cancer Institute, stresses the importance of a CT scan before radiation therapy.
Continue readingWhat is Urinary Incontinence in Women and how can Dr. Amar Raval help?
KEY TAKEAWAYS:
- Women commonly experience stress incontinence and urge incontinence, both of which can significantly impact their quality of life.
- Dr. Amar Raval offers various treatment options, including medications, Interstim devices, Botox, needle acupuncture, urethral slings, and robotic surgery.
- The Advanced Urology Institute, led by Dr. Raval, is committed to helping women improve their quality of life and confidence by addressing urinary incontinence.
Urinary incontinence can significantly impact a woman’s quality of life, causing embarrassment, discomfort, and inconvenience. Dr. Amar J. Raval, a urologist in Tampa, FL, offers various treatment options for women suffering from urinary incontinence. The Advanced Urology Institute, the largest urology practice in Florida, provides comprehensive care for women experiencing urinary incontinence and other urological issues.
Types of Urinary Incontinence in Women
Women often experience two main types of urinary incontinence: stress incontinence and urge incontinence. Stress incontinence occurs when women leak urine during activities that put pressure on the bladder, such as laughing, coughing, or sneezing. Urge incontinence involves a sudden, intense urge to urinate, followed by involuntary leakage of urine. Both conditions can be distressing and inconvenient, but treatment options are available to help manage the symptoms and improve women’s quality of life.
Treatment Options for Urinary Incontinence
Dr. Raval offers a variety of treatment options to help women manage urinary incontinence. These options include:
- Medications: Some medications can help control the symptoms of urinary incontinence, particularly urge incontinence.
- Interstim device: This device stimulates the sacral nerves, helping to regulate bladder control and reducing the symptoms of urinary incontinence.
- Botox: Injections of Botox into the bladder can help relax the bladder muscles, decreasing urinary urgency and leakage.
- Needle acupuncture: Acupuncture needles can help stimulate specific points on the body, which may help reduce the symptoms of urinary incontinence.
- Urethral slings: These surgical devices can support the urethra and help prevent stress incontinence.
- Robotic surgery: For women experiencing bladder prolapse, robotic surgery can lift the bladder and prevent further prolapse.
Improved Quality of Life and Confidence
By addressing urinary incontinence, women can experience improved confidence and quality of life. Dr. Raval and the team at the Advanced Urology Institute are dedicated to helping women regain control over their bladder and live more comfortably and confidently.
Advanced Urology Institute
The Advanced Urology Institute is the largest urology practice in Florida, providing comprehensive care for patients experiencing urinary incontinence and other urological issues. Led by experienced professionals like Dr. Amar Raval, the institute offers personalized treatment plans designed to address each patient’s unique needs and preferences.
TRANSCRIPTION:
Women generally present with issues like stress incontinence where they laugh, cough and sneeze
and leak urine or feel the urge to go don’t make it in time and leak urine and those are
big issues for them to have to wet themselves while they’re out in public and to be able
to control that with either it’s a medication or different other devices whether it’s an
interstim device, Botox or you know even a needle acupuncture needle that can have sense
to help mitigate that. I think there’s a lot of options that are available as well as for
stress incontinence, urethral slings or if they have prolapse or bladder prolapse or there’s also
robotic surgery that you can do to kind of lift the bladder up and to prevent the prolapse. So
I think from a lifestyle standpoint it makes a big difference and women are generally happier
and more confident in themselves.
REFERENCES:
- “Types of urinary incontinence – Harvard Health.” 28 Dec. 2014, https://www.health.harvard.edu/bladder-and-bowel/types-of-urinary-incontinence.
- “Urinary incontinence – Diagnosis and treatment – Mayo Clinic.” https://www.mayoclinic.org/diseases-conditions/urinary-incontinence/diagnosis-treatment/drc-20352814.
- “Urinary incontinence treatments for women (Beyond the Basics).” 16 Mar. 2022, https://www.uptodate.com/contents/urinary-incontinence-treatments-for-women-beyond-the-basics.
Side Effects with Radiation Therapy for Prostate Cancer
Key Takeaways:
- Technology advancements have made radiation therapy for prostate cancer far less daunting than it was in the past.
- Radiation therapy is non-invasive and virtually painless.
- Advanced Urology Institute in Oxford, FL offers state-of-the-art radiation therapy for prostate cancer.
Introduction: Changing Perceptions on Radiation Therapy
Radiation therapy for prostate cancer has come a long way in the past decade. Patients who have heard stories of their friends’ experiences with older treatments may be apprehensive. However, as one patient describes, “ten years ago, my buddy had this treatment, I’m real concerned that I’m going to go through the same thing.” Thankfully, they quickly learn that their treatment course will be much different, with far fewer side effects, due in large part to advances in technology.
The Treatment Experience: Simple, Pain-Free
One of the primary benefits of modern radiation therapy for prostate cancer is that the treatment is non-invasive and virtually painless. As one patient recounts, “their treatment time comes, they lay on the table, the machine rotates around them. It’s kind of like getting an x-ray. About ten minutes later, they’re done.” The hardest part, they say, is simply getting to the clinic every day. Patients undergoing radiation therapy for prostate cancer are often surprised by its simplicity and pain-free nature.
Targeted Treatment: Minimizing Side Effects
The new technology involved in radiation therapy has been developed to minimize side effects. By focusing the radiation precisely on the target area, side effects caused by radiation damage to surrounding tissues are significantly reduced. Patients treated with the latest technology are less likely to experience the same side effects as those who underwent treatment ten years ago.
Life After Treatment: A Positive Outlook
For many patients who have completed radiation therapy, the overall experience and recovery process is far more manageable than they initially imagined. After completing their first session, patients are often shocked by the ease and painlessness of the treatment, exclaiming “that’s it?” Confident in their decision to undergo radiation therapy, they can focus on their recovery and long-term health with a positive outlook.
Choosing The Right Clinic: Advanced Urology Institute
Finding the right clinic for prostate cancer treatment is essential. Advanced Urology Institute, the largest urology practice in Florida, offers state-of-the-art radiation therapy for prostate cancer. Their expert team, located in Oxford, FL, specializes in providing patients with effective, personalized treatment plans to minimize side effects while maximizing results. Choosing Advanced Urology Institute for your radiation therapy ensures that you will receive the highest standard of care and the most advanced treatment options available.
In summary, advancements in technology have made radiation therapy for prostate cancer treatment far less daunting than it might have been in the past. With cutting-edge techniques that minimize side effects and a focus on patient comfort, those undergoing radiation therapy can expect a positive, pain-free experience. For those seeking treatment in Florida, the Advanced Urology Institute is the premier choice for prostate cancer care. Their Oxford, FL location offers state-of-the-art radiation therapy backed by an expert medical team dedicated to patient success.
Transcription:
So, the patients that come in and say, 10 years ago my buddy had this treatment, I’m real concerned that I’m going to go through the same thing. They’re not going to see and experience the same side effects that a person who had treatment 10 years or later is going to have. Their treatment course is going to be a much different treatment course. Generally, the side effects using the new technology are going to be significantly less than they were with the older technology that we had. So, when patients hear that, they say, well gosh, that sounds really good. In general, radiation therapy for the most part is a painless procedure. It’s maybe some of the side effects that go along with radiation therapy depending on the target that we’re treating. For prostate cancer patients, they’re generally not going to have any side effects that are going to cause any pain. The treatment is going to be painless. The hardest thing they’re going to have to do is basically get to the clinic every day. When they get to the clinic, their treatment time comes, they lay on the table, the machine rotates around them. It’s kind of like getting an x-ray. About 10 minutes later, they’re done. The therapists come in the room and lower the patient on the table. On the first day, the patients normally say, hey, that’s it? And we say, yeah, that’s it. That’s all we have to do. So, they’re generally surprised about the non-invasive, painless treatment that radiation therapy gives.
What is the first sign of bladder cancer? with Dr. Ketan Kapadia
KEY TAKEAWAYS:
- The first sign of bladder cancer is often gross hematuria, or visible blood in the urine.
- Early detection of bladder cancer is crucial for more effective treatment and improved patient outcomes.
- The Advanced Urology Institute, led by Dr. Ketan Kapadia, offers comprehensive care and state-of-the-art treatments for patients with bladder cancer and other urological issues.
Bladder cancer is a common type of cancer that affects many individuals, particularly those with a history of smoking. Dr. Ketan A. Kapadia, MD, a board-certified urologist in St. Petersburg, FL, discusses the early signs of bladder cancer and the importance of early detection for effective treatment. The Advanced Urology Institute provides comprehensive care for patients dealing with bladder cancer and other urological issues.
First Sign of Bladder Cancer: Gross Hematuria
According to Dr. Kapadia, the most common and critical first sign of bladder cancer is gross hematuria, or visible blood in the urine. This symptom should be taken seriously, as it could indicate the presence of bladder cancer, particularly among individuals with a history of smoking. Even for those who have quit smoking, the risk of bladder cancer remains elevated.
The Importance of Early Detection
Dr. Kapadia emphasizes the importance of catching bladder cancer in its early stages, as this allows for more effective treatment and a better prognosis. If a patient experiences urinary complaints such as blood in the urine or more frequent urination, they should be evaluated for bladder cancer. Early detection and diagnosis can lead to more conservative treatments and improved outcomes for patients.
Bladder Cancer and Smoking
Smoking is a significant risk factor for bladder cancer, with former and current smokers being at higher risk. Dr. Kapadia notes that even after quitting smoking, individuals remain at an elevated risk for developing bladder cancer. This highlights the importance of regular screenings and evaluations for those with a history of smoking, as early detection is critical in bladder cancer treatment.
Treatment Options for Bladder Cancer
In the past, cystectomies, or the surgical removal of the bladder, were a common treatment for bladder cancer. Dr. Kapadia, who trained with leading expert Donald Skinner, has extensive experience in performing cystectomies and bladder reconstruction. However, thanks to advances in medical knowledge and treatment options, bladder removal is now less common. By catching bladder cancer early, more conservative treatments may be possible, resulting in better outcomes for patients.
Advanced Urology Institute
As the largest urology practice in Florida, the Advanced Urology Institute offers comprehensive care and state-of-the-art treatments for a wide range of urological issues, including bladder cancer. Dr. Ketan Kapadia and his team of experienced professionals are dedicated to providing personalized care and innovative solutions for patients, with a focus on early detection and effective treatment options.
TRANSCRIPTION:
I’m Ketan Kapadia, I’m with Advanced Urology Institute and board certified urologist.
Well number one is gross hematuria, blood in the urine.
If you see blood in the urine we need to make sure you don’t have bladder cancer and obviously
we see a lot of bladder cancer in Florida.
It happens to be much increased on patients who’ve had smoking history, even if you quit
you’re still at risk.
I used to do a lot of cystectomies where we removed bladders and do reconstruction.
Fortunately we don’t have to do those as much anymore.
I trained with Donald Skinner who was the leading expert on doing that operation.
But again we want to try to catch things early.
If somebody’s having urinary complaints of blood or even just more frequently going to
the bathroom and things are not right that may need to be evaluated for bladder cancer.
How does Dr. Rishi Modh treat female urinary incontinence?
KEY TAKEAWAYS:
- Urinary incontinence, a common condition among women, should not be accepted as a normal part of aging.
- Dr. Rishi Modh, a urologist in St. Petersburg, FL, offers a variety of treatment options for female urinary incontinence, including medications and procedures.
- The Advanced Urology Institute, the largest urology practice in Florida, provides comprehensive care and state-of-the-art treatments for women experiencing urinary incontinence.
Urinary incontinence is a condition that affects many women, and it is often mistakenly considered a normal part of aging. Dr. Rishi Modh, MD, MBA, a board-certified urologist in St. Petersburg, FL, challenges this misconception and highlights the various treatment options available for female urinary incontinence. Dr. Modh and the team at the Advanced Urology Institute work to improve the quality of life for women experiencing this condition.
Understanding Female Urinary Incontinence
While urologists are often associated with treating male patients, Dr. Rishi Modh emphasizes that they also treat numerous women for various urological issues, including urinary tract infections (UTIs) and urinary incontinence. Urinary incontinence, or the involuntary leakage of urine, is a common condition among women that can significantly impact their quality of life.
Challenging the Misconception
Dr. Modh stresses that urinary incontinence should not be accepted as a normal part of aging for women. Instead, women experiencing this condition should seek medical help, as there are various treatment options available to address and improve urinary incontinence. The goal is to enable women to live their lives without the discomfort and embarrassment associated with involuntary urine leakage.
Treatment Options for Female Urinary Incontinence
At the Advanced Urology Institute, Dr. Rishi Modh offers a range of treatment options for female urinary incontinence. These options include medications and procedures tailored to address the specific type of incontinence a patient is experiencing. By offering individualized care and evidence-based treatments, Dr. Modh and his team can significantly improve the quality of life for women suffering from urinary incontinence.
Advanced Urology Institute
The Advanced Urology Institute is the largest urology practice in Florida, providing comprehensive care and state-of-the-art treatments for a wide range of urological issues. With a team of dedicated and experienced professionals, the Institute is committed to offering innovative solutions and personalized care to patients experiencing urinary incontinence. Women seeking help for urinary incontinence can trust the expertise and compassionate care provided by Dr. Rishi Modh and the Advanced Urology Institute.
TRANSCRIPTION:
My name is Rishi Modh, I’m a board-certified urologist with Advanced Urology Institute.
Most commonly people think of a urologist as treating guys, but we treat numerous women for a whole host of problems. The most common problems being issues with urinary tract infections and urinary leakage. So unfortunately a lot of women accept urinary incontinence or leaking urine as a normal part of being a woman and getting older.
This does not have to be the case. We have great treatment options for medications to procedures for all different types of incontinence and we can really make a difference in people’s quality of life.
REFERENCES:
- “Urinary Incontinence in Women | Johns Hopkins Medicine.” https://www.hopkinsmedicine.org/health/conditions-and-diseases/urinary-incontinence/urinary-incontinence-in-women.
- “What’s the Treatment for Urinary Incontinence in Women? – WebMD.” 20 Apr. 2021, https://www.webmd.com/urinary-incontinence-oab/treatment-urinary-incontinence-women.
- “Common Female Urology Problems and How to Treat Them.” 6 Apr. 2017, https://www.michiganmedicine.org/health-lab/female-urologist-explains-womens-most-common-urological-concerns-and-how-treat-them.
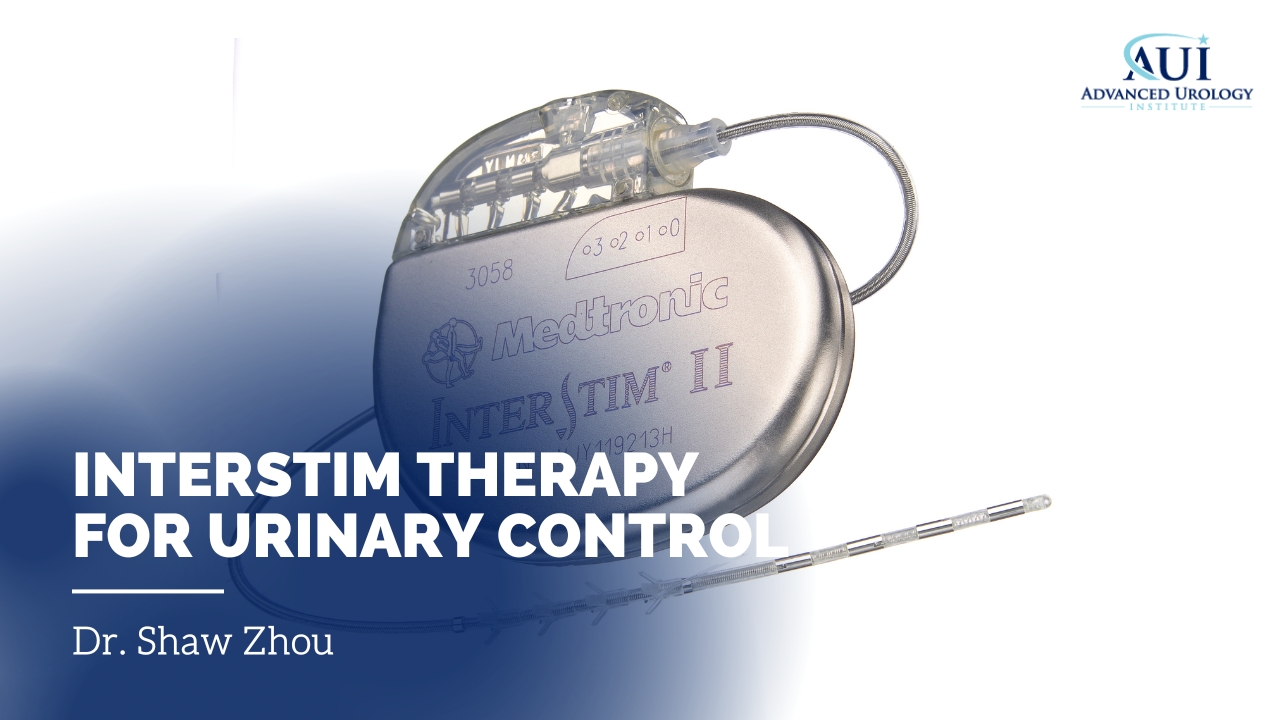
What is Dr. Shaw Zhou’s approach to InterStim Therapy for Urinary Control?
KEY TAKEAWAYS:
- Dr. Shaw Zhou is a leading urologist in St. Petersburg, FL, specializing in InterStim Therapy for urinary control.
- InterStim Therapy has evolved over the years, becoming smaller and more refined, making it an increasingly effective treatment option for urinary incontinence and urinary retention.
- Dr. Zhou’s innovative high-frequency programming technique has the potential to revolutionize InterStim Therapy, reducing the need for medication and offering a sustainable, effective solution for urinary control.
InterStim Therapy is a proven and innovative treatment for urinary retention and urinary incontinence. Dr. Shaw W. Zhou, MD, FACS, a leading urologist in St. Petersburg, FL, has been working with this technology for over 17 years. In this article, we will explore Dr. Zhou’s approach to InterStim Therapy, how the device has evolved over the years, and the future prospects of this treatment for urinary control.
InterStim Therapy Explained
InterStim Therapy is a minimally invasive treatment that utilizes a small device to stimulate sacral nerves. This FDA-approved therapy is designed to help patients who suffer from urinary retention or urinary incontinence. Dr. Shaw Zhou, a urologist at the Advanced Urology Institute, has witnessed firsthand the evolution of this technology and has participated in clinical trials to further advance its effectiveness.
The Evolution of InterStim Therapy
Over the past 17 years, Dr. Zhou has observed the continuous advancement of InterStim Therapy devices. In the beginning, the devices were bulky and less user-friendly. However, they have since become smaller and more refined, similar to the progression of cell phones from earlier models to the current iPhone series.
Innovative High-Frequency Programming
Recently, Dr. Zhou has been working on a new high-frequency programming technique that allows the device to stimulate sacral nerves at an astounding rate of 10,000 times per minute. This new approach is currently being tested in clinical trials, and the results so far have been extremely encouraging.
The Future of InterStim Therapy for Urinary Incontinence
Dr. Zhou is confident that InterStim Therapy will be the future for treating urinary incontinence. He believes that as the technology continues to advance, patients will no longer need to rely on medication for their urinary control issues. This groundbreaking therapy offers a more sustainable and effective solution that has the potential to significantly improve the quality of life for countless individuals.
Advanced Urology Institute
The Advanced Urology Institute is the largest urology practice in Florida, offering state-of-the-art treatments and cutting-edge technology to address a wide range of urological concerns. With a team of experienced and dedicated professionals, the Institute is committed to providing the highest quality of care for their patients. For those considering InterStim Therapy, the Advanced Urology Institute is an excellent choice for leading expertise and innovative solutions in the field of urology.
TRANSCRIPTION:
My name is Shaw Zhou. I’m with the Advanced Urology Institute. Interesting is with a device
we put in to stimulate sacral nerves so it works FDA-proof for either urinary retention
or urinary incontinence. It’s extremely amazing, this device. Just like other technology. Now
we can have a new program we’re doing with high frequency. We can stimulate 10,000 times
a minute. We’re doing a clinical trial. So far results are very encouraging. I’ve been
doing this for 17 years but the device keeps on advancing. Just like your cell phone. You
got iPhone 10 now. You know what I’m saying? So you got when I start doing a big bulky
device now become a smaller, smaller. We provide numerous programs. We have higher frequency. So it’s extremely encouraging. I think it will be the future for the urinary incontinence because that way you don’t need to take medication no more.
REFERENCES:
- “InterStim Therapy for Bladder Control – SSM Health.” https://www.ssmhealth.com/conditions-treatments/urology/interstim-therapy-for-bladder-control-problems.
- “InterStim Implants for Urinary or Bowel Incontinence.” https://myconfidentlife.com/treatment-options/interstim.
- “Sacral Neuromodulation | Medtronic.” https://www.medtronic.com/us-en/healthcare-professionals/therapies-procedures/urology/sacral-neuromodulation.html.
Urology Tests and Procedures with Chad Bryan PA-C
Chad Bryan, a physician assistant for Advanced Urology Institute, discusses the importance of understanding prostate health in men. He highlights how society is becoming more educated about the issue through direct advertising from pharmaceutical companies.
Continue readingBecoming a Physician Assistant with Chad Bryan PA-C
Becoming a PA requires a significant amount of education and experience, but for those who are dedicated to the profession, it can be a rewarding and fulfilling career choice.
Continue readingGuidelines for Treating Prostate Cancer with Dr. Bill Vanasupa
Dr. Billy Vanasupa talks about the importance of informed decision-making when it comes to prostate cancer treatment. While medical professionals can offer guidance and recommendations based on the latest research and guidelines, ultimately, the patient should have a say in their treatment plan.
Continue readingPenile prosthesis for the management of Peyronie’s disease – Dr. Arash Rafiei
Penile prosthesis are a valuable treatment option for men with ED and Peyronie’s disease who have not responded to other treatments. While the placement of a penile prosthesis can be more difficult in cases where there is curvature or scarring present, most patients will see positive results over time.
Continue reading