Drs. Jay and Bassel, board-certified urologists in Naples and Palm Harbor, FL, respectively, talks about addressing common female urology problems.
Continue readingJanelle Bunce, PA-C: Why Advanced Urology Institute?
“AUI is a phenomenal single specialty practice where we can really focus on urology.” says Janelle Bunce, a physician assistant in Naples, FL
Continue readingThe Impact of Radiation Therapy in Urological Care
Our urologists in Naples and Largo, FL provides a foundation for understanding the impact of radiation therapy in the realm of urology.
Continue readingUnparalleled Urology Care Awaits You at Naples Office
At our Naples Office, you’ll find an exceptional lineup of accomplished urologists and providers dedicated to patient care.
Continue readingWhat Female Urology Conditions Can Dr. Jonathan Jay Treat?
How Did Dr. Rolando Rivera Become a Urologist?
What does a physician assistant do According to Janelle Bunce?
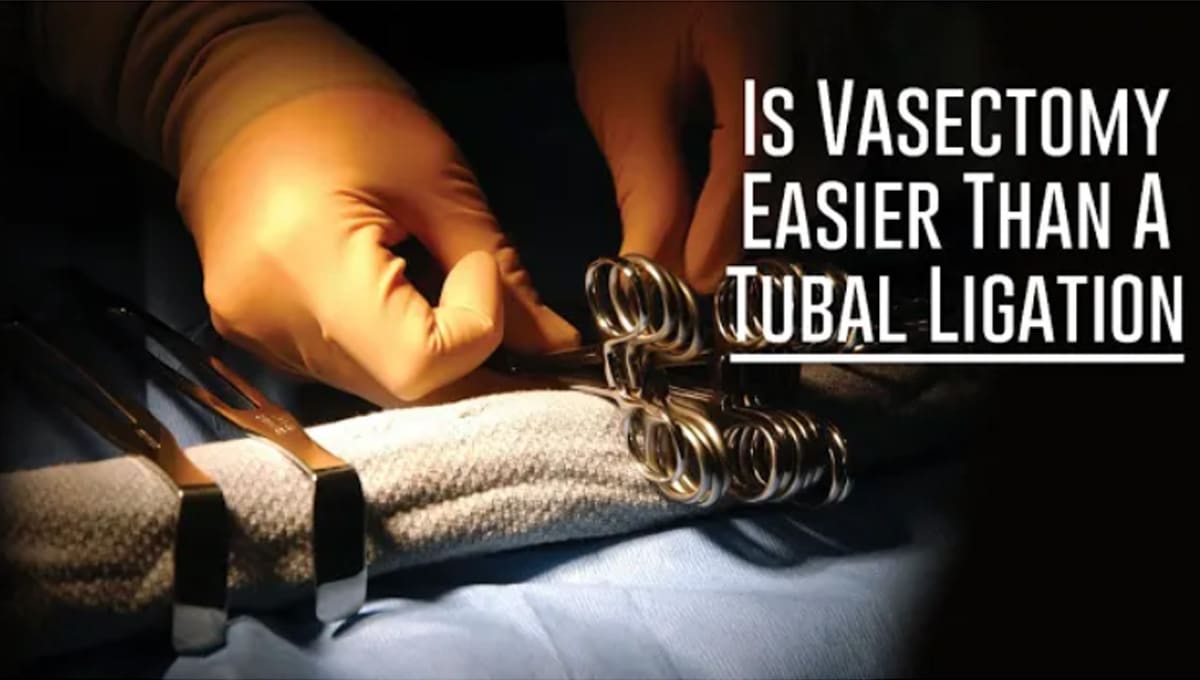
Is Vasectomy Easier Than A Tubal Ligation
Both a vasectomy and tubal ligation are minor surgical procedures done to prevent pregnancy. A vasectomy is performed on men. During the procedure, the vas deferens, which are the two tubes through which sperm is transported into the ejaculatory duct during ejaculation, are cut or closed off to prevent the release of sperm when a man ejaculates.
Tubal ligation is the equivalent of vasectomy for women. It involves cutting or sealing off the fallopian tubes. The fallopian tubes are the path through which the egg produced by the ovaries travels to the womb. When the tubes are cut or sealed, the egg cannot travel to meet the sperm. This means that fertilization never happens and no pregnancy results.
Comparing Vasectomy and Tubal Ligation.
1. Procedure
 During a vasectomy,the urologist makes two tiny incisions on the scrotum, pulls out the vas deferens and snips them and ties the individual ends. For tubal ligation, the doctor makes an incision in the patient’s abdomen to reach the fallopian tubes. The tubes are then cut and closed off. Or the tubes can be left uncut and closed off using a clip or a band.
During a vasectomy,the urologist makes two tiny incisions on the scrotum, pulls out the vas deferens and snips them and ties the individual ends. For tubal ligation, the doctor makes an incision in the patient’s abdomen to reach the fallopian tubes. The tubes are then cut and closed off. Or the tubes can be left uncut and closed off using a clip or a band.
While both procedures qualify as minor surgeries, a tubal ligation is a little more invasive. It involves larger incisions and the risk of interfering with other internal organs is significantly higher. On this score, a vasectomy seems a better option.
2. Cost of Procedure
Tubal ligation takes longer. It takes more work to complete than a vasectomy. Additionally, a tubal ligation requires the use of general anaesthetic to a greater extent than a vasectomy. For these reasons, it is more expensive.
3. Risks and Side Effects
Although both procedures have side effects, it must be said that serious complications rarely arise from either procedure.
A vasectomy may cause some bleeding and a little pain in the scrotum. There is a risk of infection but because the incisions are usually so small, the risk is minimal. A tubal ligation, on the other hand, has an increased risk of infection. There is also a greater risk of injury to internal organs because fallopian tubes are located inside the body, unlike the scrotum. After the surgery, the woman may have bleeding in the abdomen.
Based on the general criteria, vasectomy is said to be preferred to a tubal ligation. The choice, however, should always be made by the couple involved after they have weighed the choices and their personal circumstances. The advice of a trained urologist can help make the decision process easier. The staff of experts at Advanced Urology Institute are experienced in helping with consultations, planning and doing both procedures. For more information, visit the Advanced Urology Institute website.
What Procedures Are Performed in the New AUI Surgery Center?
Advanced Urology Institute offers a wide range of outpatient urology procedures in every new surgery facility. Whenever possible, there is a preference for treating patients in outpatient settings where primary, less complicated interventions are provided by board-certified urologists and other skilled medical professionals. Patients have the same quality of care they would get at a hospital setting at a lower cost. And with increased availability of advanced medical technology for outpatient care, new surgical centers have ensured redistribution of procedures and improved the efficiency of delivery of services.
Large number of procedures
At AUI, new surgery centers are used for a large number of procedures, including simple reconstructive operations, stone disease, scrotoplasty, meatoplasty, orchiopexy, pelvic prolapse, prostate and bladder procedures. For instance, urologists at new surgery centers treat incontinence, hematuria, kidney stones, urethritis, inguinal hernia, hydrocele, prostatitis, BPH, urinary tract trauma, urethral strictures, inflammatory urinary tract and bladder diseases, and urinary tract infections. And the fact that the centers are found in different locations encourages redistribution of care and access by more patients.
Common procedures performed in new AUI centers include:
- Prostate biopsy: Sampling of diagnostic tissue to be used to test for cancer cells.
- Bladder biopsy: Removing or sampling of tissue from the lining of the bladder.
- Ureteroscopy: Removing kidney stones using thin telescopic instruments
- Cystoscopy: Using a tiny camera to examine an affected area in the bladder through the urethra.
- Lithotripsy: Using shock waves to break down kidney stones.
- Penile prosthesis: Implanting a device in the penis to treat erectile dysfunction.
- Vasectomy for male sterilization.
- Circumcision: Removing some or all prepuce (foreskin) from the penis.
- Incontinence sling procedure: Implanting an internal support to the urethra to lift it to the normal position and treat incontinence.
- Laser vaporization or transurethral resection of prostate: Using a tiny instrument with a laser or electrical loop inserted into the penis to help remove obstructing tissue.
- Brachytherapy: Treating prostate cancer by inserting radioactive “seeds” directly into the tissues harboring the cancerous tumor.
- Hypospadias: Reconstructing a straight penis, making its urethral opening as close to the penis tip as possible.
- InterStim (sacral nerve stimulation): Implanting a tiny pacemaker near the tailbone.
- UroLift: Procedure to lift or hold the enlarged prostate tissue out of the way to prevent blockage of the urethra.
- Botox injection: Injecting Botox directly into bladder muscles.
For the more complex procedures that require special equipment, patients are usually admitted to the hospital. For example, robotic surgery procedure, pyeloplasty (reconstruction of renal pelvis), nephrectomy, ureteral reimplants and ureteral stent placement are conducted in hospital settings.
At Advanced Urology Institute, we are committed to delivering top-notch urological care to all our patients. Our surgeons are fully-qualified, board-certified, fellowship-trained urologists, who are renowned for their exceptional expertise in treating urological problems. We also have surgical centers that are supplied with the latest medical equipment and technologies to provide the best possible care.
For more information about our urological services, visit the Advanced Urology Institute website.
Female Pelvic Medicine and Reconstructive Surgery at AUI
Treatment Options Available for Pelvic Organ Prolapse
A pelvic organ prolapse involves the drooping of pelvic organs due to a weakness in the muscles of the pelvic floor. When this happens, the bladder, the small intestine, the rectum, the uterus or the upper vaginal wall drops into the vagina. The condition disrupts the urine flow and can affect the reproductive function by making it difficult, uncomfortable or painful to have sexual intercourse.
The condition can be treated by:
1. Physical exercise
Kegel exercises can strengthen pelvic muscles. The exercises involve a woman imagining she has to urinate, then instead of letting it out, she squeezes her muscles to hold it in. It is recommended to repeat the exercises 10 to 15 times a day.
2. A pessary
This is a ring-like device that is inserted into the vagina to hold the affected organ in its proper place.
3. Pelvic Reconstructive Surgery
 Reconstructive surgery is a testimony to how much technology has improved the practice of medicine. In cases of pelvic organ prolapse, the surgery is performed to restore the affected organ to its proper place. There are different types of reconstructive surgery, depending on the type of organ prolapse being treated. Whatever the type of reconstructive surgery, however, it is a minimally invasive procedure.
Reconstructive surgery is a testimony to how much technology has improved the practice of medicine. In cases of pelvic organ prolapse, the surgery is performed to restore the affected organ to its proper place. There are different types of reconstructive surgery, depending on the type of organ prolapse being treated. Whatever the type of reconstructive surgery, however, it is a minimally invasive procedure.
Even though it is effective, not every patient qualifies for reconstructive surgery. Some factors that must be considered include:
- When a woman intends to have children. The surgery may be discouraged because the prolapse may return after the birth.
- Age. Younger women may be advised not to have the surgery because of the risk that it may recur and they are more likely to have a child in the future, increasing the risk of a recurrence.
- When one has a serious illness, it may be advisable not to have the surgery so as to avoid complications.
The well being of the patient is a top priority at AUI. A female patient with organ prolapse will not only receive the most advanced treatments available, the team also will listen to her questions and work with her on a plan of treatment that is best suited to her needs. AUI makes it a priority to provide information on the topic of pelvic organ prolapse and to be available to discuss any concerns. For more information, visit the Advanced Urology Institute website.
Are Enlarged Prostate and Urinary Problems Common?
Normal part of aging
Just like gray hair, BPH is a natural result of getting older. But the trouble is, it is characterized by nightly trips to the bathroom which may become too frequent and eventually disrupt daytime routine. In some cases, an enlarged prostate may make it difficult for you to sit through a plane flight or meeting without getting up. So it can be a really annoying problem.
How does BPH occur?
As men grow older, the prostate gland becomes bigger with cells multiplying gradually and creating an enlargement that exerts pressure on the urethra. Since urine flows from the bladder through the urethra in men, an enlarged prostate blocks urine flow. With increased pressure on the urethra, the bladder is compelled to contract more forcefully to push urine through the body. With time, the bladder muscles become thicker, stronger and overly sensitive, beginning to contract even when only a small amount of urine is inside and triggering the need to pass urine frequently.
Eventually, bladder muscles fail to overcome the effect of a narrowed urethra and cannot empty all the urine. That means some urine is left inside the bladder every time after urination. When the bladder is continuously not emptied completely, there is an increased risk of urinary tract infections. Incomplete emptying also can lead to serious problems over time, including incontinence, blood in urine, bladder stones and acute urinary retention (the inability to urinate). In rare cases, incomplete emptying of the bladder may cause bladder damage or even kidney damage.
Symptoms of BPH include:
- Frequent urination
- Urgent urination
- Nocturia (frequent urination at night)
- Trouble starting urination
- Weak urine stream
- Urine stream that stops and starts
- Straining to urinate
- Inability to empty bladder completely
- Returning to the bathroom to urinate a few minutes after urinating
- Dribbling at the end of urination
In rare cases, signs of BPH also may include:
- Blood in urine
- Inability to urinate
- Urinary tract infection
A sudden and complete loss of ability to urinate is a medical emergency so you should see a urologist immediately. But you also should see a doctor whenever you are experiencing urinary symptoms, even if they are not really bothersome. Such visits to the doctor will ensure that the underlying causes of your condition are identified or ruled out. Remember that undiagnosed and untreated urinary problems may cause complete obstruction of the urinary tract, bladder and kidney damage and other serious problems.
At Advanced Urology Institute, we offer several safe and effective treatments for urinary problems. For instance, if you have BPH, we may:
- Offer a long course of antibacterial medication to treat bacterial prostatitis.
- Provide medication to improve your urine flow and relieve symptoms.
- Perform surgical procedures such as:
-
-
- (a) Transurethral resection of your prostate (TURP).
-
- (b) Transurethral incision of your prostate (TUIP).
-
- (c) PVP (green light laser resection) or HoLEP (holmium laser resection) of prostate.
-
- (d) Open prostatectomy for very large prostates.
-
- (e) Urolift (transurethral insertion of clips to separate prostate lobes).
-
- (f) Aqua-ablation (removal of prostate tissue with water jets).
- (g) Rezum therapy (removal of prostate tissue with steam).
-
So you don’t have to suffer embarrassing urinary symptoms when you have BPH. At AUI, we can fix your condition and enable you to live your life with freedom and confidence. For more information on our treatment options for BPH and other urinary problems, visit the Advanced Urology Institute website.
What is Erectile Dysfunction and How to Treat it?
Erectile dysfunction is the inability to have or maintain an erection firm enough for sexual intercourse. Any man may find himself occasionally unable to achieve an erection. That is normal. It is only when this inability becomes a sustained everyday occurrence that he may consider the possibility of erectile dysfunction.
The main factor for erectile dysfunction is aging, starting about the age of 50. Over 50 percent of men over 50 suffer from erectile dysfunction. Other risk factors include cardiovascular disease, high blood sugar, high blood pressure and high cholesterol levels. Emotional and mental conditions such as depression and anxiety also can cause erectile dysfunction.
Treating Erectile Dysfunction
Men who suffer from erectile dysfunction have a number of treatment options. If it is a symptom of an underlying illness, treatment should be focused on the underlying illness. When erectile dysfunction appears with no underlying cause, the following treatment options are available and are highly successful.
1. Oral Medication. These are pills given to increase blood flow to the penis, thus causing an erection. The most common ones are vardenafil or Levitra, Cialis or tadalafil, viagra and avanafil. Oral medication is most successful in patients with mild cases of erectile dysfunction.
2. Penile injections. The most common injectible drug is alprostadil. Using a very fine needle, a patient injects the drug into the base of the penis. The drug increases the size of the arteries that supply blood to the penis. Alprostadil also can be administered by placing a small alprostadil suppository at the opening of the penis, rather than by injection.
3. Vacuum erection device. This is a tube with a hand or battery powered pump. The tube is placed over the penis and the pump is used to draw air out, creating a vacuum. The vacuum thus draws blood into the penis, causing an erection.
4. Penile implants. A minor surgical procedure is used to introduce bendable rods at the sides of the penis. These rods give the penis a firmness that allows for intercourse. An alternative of the rods is the insertion of fluid filled cylinders connected to a pump placed in the scrotum. Engaging the pump inflates the cylinders which causes the penis to firm up.
It is advisable for men, especially those approaching age 50, to maintain a healthy relationship with a urologist. An experienced urologist can diagnose and offer advice on the best treatment options. It is also important to stay informed on the causes, signs and symptoms of erectile dysfunction. Many professional sites, such as the one maintained by the Advanced Urology Institute, are very helpful. Advanced Urology Institute also has an experienced team of specialists who can help with consultation, diagnosis and treatment. For more information, visit the Advanced Urology Institute website.
What are the advantages of the da Vinci surgical system?
The da Vinci surgical system is an advanced and effective tool for performing minimally-invasive surgeries. It is a state-of-the-art tool that makes the most of the surgeon’s skill, expertise and experience in conducting urologic procedures. Known as da Vinci because Leonardo da Vinci devised the first robot and used three-dimensional detail and incomparable anatomical accuracy to give life to his masterpieces, the surgical system gives physicians such precision and detail that it effectively simulates an open surgical environment while allowing the use of tiny incisions.
How does the da Vinci system work?
The da Vinci surgery is robot-assisted and minimally-invasive, done via small incisions. The robot’s hands offer a high degree of dexterity, which enables surgeons to operate in the very tight spaces and delicate tissues of the genitourinary tract that otherwise would only be accessed through the longer incisions of open surgery. The da Vinci robot is a self-empowered, computer-controlled device that has been programmed to help in the positioning and maneuvering of surgical instruments. It gives surgeons better precision, flexibility, accuracy and control over surgical procedures.
When using the da Vinci system:
1. The urologist operates from a computer console situated in the operating room, directing and manipulating miniaturized instruments mounted on 3 robotic arms to create small incisions in the patient.
2. During the procedure, the doctor looks through a 3D camera attached to a fourth robotic arm that magnifies the surgical site.
3. The hand, wrist and finger movements of the surgeon are transmitted straight through the computer console and to the instruments attached to the robotic arms, resulting in mimicked movements with the same range of motion as that of the surgeon and allowing maximum control.
4. The robot is supervised by the surgical team at the patient’s bedside.
What are the advantages of the da Vinci surgical system?
1. It ensures that surgeries are more precise by providing better visualization, improved dexterity and greater accuracy.
2. It enables surgeons to conduct complex surgical procedures using tiny incisions.
3. It replicates the surgeon’s technique and movements in real-time, with the surgeon seated just a feet away from the patient viewing an actual image of the operating field while performing the procedure in real-time by manipulating a miniaturized instrument and using tiny incisions.
4. It transmits force feedback sensations from the operating field to the surgeon, which are then used as a substitute for tactile sensations and are augmented by the superior vision offered by the high-resolution 3D view to deliver better visualization, accuracy and precision.
The da Vinci is designed to ensure that both simple and complex procedures are done using incisions of 1-2 cm (also called operating ports), potentially resulting in:
1. Reduced trauma, pain and discomfort to patients
2. Fewer complications
3. Shorter recovery time and quicker return to routine activities
4. Minimal scarring
5. Reduced blood loss and need for transfusions
6. Minimal hospitalization costs
At Advanced Urology Institute, we have incorporated the da Vinci surgical system into our practice. Over the years, we have been able to use the increased range of motion, improved visualization, enhanced dexterity and greater surgical precision offered by the robotic system to deliver improved treatment outcomes to our patients. We are also proud of the skilled and experienced professionals at AUI whose training, fortitude, passion and expertise in the use of advanced technologies have enabled us to provide the best possible care to our patients. For more information on our services, visit the “Advanced Urology Institute” site.
Ways to Treat Erectile Dysfunction
If you suspect that you have erectile dysfunction, you need to talk to your doctor about it. Then you can work with the doctor to determine the underlying factor or cause of the condition. Actually, ED can only be effectively treated if what is causing it is known. In fact, you may find that your condition improves with only simple lifestyle changes, such as losing weight, quitting smoking or drinking less alcohol. And if it is a medication you’re taking that is causing the problem, your doctor may treat the condition by reducing the dosage or having you try another drug.The treatment options for ED include lifestyle changes, counseling, medications, penile injections, vacuum pumps and surgery.
1. Lifestyle changes
Making lifestyle changes can reduce the severity or improve erectile dysfunction. Some of the changes are:
a. Quitting smoking
b. Stopping or reducing alcohol consumption
c. Increasing physical activity or exercise
d. Cutting down body weight
e. Stopping the use of illegal drugs
2. Seeing a counselor
Your urologist may recommend that you see a counselor if your erectile dysfunction is worsened by psychological or emotional issues. In many cases, counselors require that you go with your partner to the counseling sessions so she can know how best to support you. And as you work on the anxiety and stress issues with your counselor, your urologist will be focused on treating any underlying physical issues. Usually only a handful of sessions with the counselor will be enough for you to overcome ED.
3. Medication
The first treatment that your urologist will offer to treat ED is oral pills. Common oral medications for ED include:
a. Sildenafil (Viagra)
b. Tadalafil (Cialis)
c. Vardenafil (Levitra or Staxyn)
d. Avanafil (Stendra).
These medicines work by relaxing your smooth muscles and increasing blood supply to the penis following sexual stimulation. You’ll be required to take them anywhere from 15 minutes to 36 hours before sex, depending on the particular drug your doctor has prescribed. Vardenafil (Staxyn) dissolves in the mouth, but the other pills are swallowed. However, you aren’t allowed to take any of these drugs more than once per day. The drugs are effective in about 80 percent of men who use them, although if you have an erection that lasts beyond 4 hours, you should seek emergency medical help.
You should not take these medicines as treatment for ED if you are already taking nitrates for a heart disorder. Since nitrates also relax and widen blood vessels, their combination with these drugs leads to a sudden reduction of your blood pressure, which may cause falling, fainting or dizziness and possible injuries. Likewise, if you are already taking drugs to treat enlarged prostate (BPH), inform your doctor about them. A combination of BPH medications called alpha-blockers with ED medicines also may result in sudden reduction of your blood pressure.
In case your erectile dysfunction is due to low testosterone levels, the urologist may prescribe testosterone. However, testosterone therapy won’t work for you if you have nerve or circulatory problems. So you must be very open with your urologist about your other medical problems before you are given any medications.
4. Penile injections
Injecting the penis with a drug called alprostadil can trigger a stronger and firmer erection. While oral medications are able to cause an erection after sexual stimulation, you can’t get an automatic erection with them. That’s why your doctor may at times opt for injecting a drug into the penis to ensure you achieve erection automatically even without sexual stimulation.
5. Vacuum constriction devices (pumps)
Vacuum pumps pull blood into the penis, resulting in an erection. A typical vacuum device is an external pump supplied with a band that you can use to achieve and maintain an erection. According to several studies, up to 50-80 percent of men who have used vacuum erection devices are pleased with the results.
A vacuum device has three components:
a. A plastic tube (cylinder), which you place toward the end of your penis.
b. A pump, which drives out air from the tube in order to create a vacuum.
c. An elastic ring (band), which you place on the cylinder, on the other end applied to your body, and then move it from the tube to the penis in order to maintain erection.
To use the vacuum erection device, you place the pump over your penis and pump out air from the tube (cylinder) to create a vacuum. The vacuum then pulls blood into the penis’ shaft and makes the penis longer and firmer. Once the penis is erect, and with the help of a lubricant, you slide the retaining band downward onto the lower end of your penis. You also remove the pump once you have released the vacuum.
The elastic ring sustains the erection by stopping blood from moving back into the body during intercourse. So you can only attempt intercourse with the elastic ring in place. And the ring can be left in place for about 30 minutes to enable successful intercourse.
6. Penile prosthesis (Penile implant surgery)
Another option for treating ED is penile prosthesis in which your urologist performs an operation to implant either a malleable (bendable) device or inflatable device into your penis. A penile implant surgery is preferred when you have an obvious medical condition that is causing the ED and the urologist is sure that your condition won’t resolve naturally or with medications.
Usually, the simplest form of penile prosthesis is surgical implantation of malleable rods inside the erection chambers of your penis. Once implanted, the rods ensure that your penis is maintained in semi-rigid state and just requires lifting or adjusting to erect position for sexual intercourse. Malleable rods are a good option if you’ve had spinal injury or have limited hand strength.
Alternatively, your doctor may go for a hydraulic, inflatable implant. With this prosthesis, you can choose to get an erection when you need to. Inflatable implants increase the size of the penis through a pump that’s located in the scrotum. The advantage of an inflatable implant over malleable rods is that the erection is more natural and easier to conceal than one achieved with malleable rods.
Penile implant surgery takes about one hour to complete and is usually performed in an outpatient setting. Following penile implant surgery, you’ll be able to leave the hospital the same day after surgery and can resume sexual intercourse 4-6 weeks after the procedure.
7. Artery reconstruction (Vascular reconstructive surgery)
Artery reconstruction is often a last resort treatment for ED because the procedure is costly, technically difficult and does not usually work. But the aim of the procedure, when recommended, is to boost blood flow in your penis and help you achieve an erection. During the operation, the urologist transfers an artery in another part of your body (usually from a muscle in the belly) to one in your penis, creating a path for blood to move around the blocked (affected) area. The procedure is only rarely considered, but may be an option for men younger than 30 who have ED because of injuries to their penis or the area around it.
Want to find out more about erectile dysfunction? Visit the “Advanced Urology Institute” site.








 One of the inevitable consequences of aging in women is urinary problems. With increasing age, the pelvic floor muscles—a group of muscles that support
One of the inevitable consequences of aging in women is urinary problems. With increasing age, the pelvic floor muscles—a group of muscles that support 
 Becoming a urologist requires a special kind of person. Urology is one of the more challenging specialties a doctor can choose. Urological problems are broad and can encompass issues ranging from urinary incontinence, overactive bladder, vaginal prolapse and kidney stones to the advanced realm of pelvic surgery. Urologists are required to have a large skill set in order to take care of their patients.
Becoming a urologist requires a special kind of person. Urology is one of the more challenging specialties a doctor can choose. Urological problems are broad and can encompass issues ranging from urinary incontinence, overactive bladder, vaginal prolapse and kidney stones to the advanced realm of pelvic surgery. Urologists are required to have a large skill set in order to take care of their patients.







 My curiosity led me to study physiology — the study of how the body works — to learn more about the body. So I attended Michigan State University to pursue a Bachelor of Science degree in physiology. As I was studying physiology, I became interested in medicine. Upon graduation, I went to Ann Arbor, University of Michigan for my medical education. After that, I moved to Henry Ford Hospital for my residency training before going to and completing my fellowship training at the Beth Israel Deaconess Medical Center.
My curiosity led me to study physiology — the study of how the body works — to learn more about the body. So I attended Michigan State University to pursue a Bachelor of Science degree in physiology. As I was studying physiology, I became interested in medicine. Upon graduation, I went to Ann Arbor, University of Michigan for my medical education. After that, I moved to Henry Ford Hospital for my residency training before going to and completing my fellowship training at the Beth Israel Deaconess Medical Center.